Since the American Recovery and Reinvestment Act (ARRA) was enacted in 2009, many healthcare providers have switched their paper records to electronic ones. This has been a major development in healthcare in general and is expected to be an improvement in health information technology in particular. Since then, the healthcare sector has seen a massive IT boom.
So, in this digital era, every healthcare provider can agree that computer systems in their IT department play a crucial role in their operation.
The computer system is set up to allow the staff to track, manage, and monitor patients’ data and communicate and connect with various entities, from insurance providers to data storage systems to referring physicians.
Therefore, every staff member (regardless of their positions) should be fully aware and have a solid understanding of how the computer system works all together to support their team and the patients they serve.
In other words, interoperability is a matter of importance for every healthcare provider.

Photo by Mart Production on Pexels
What Is Interoperability In Healthcare?
Many blog articles or healthcare explainer videos have talked about this advanced technology, but many people still have no clue about what it actually is. So, we will break down interoperability for you in a light-hearted way.
The amount of data in the healthcare ecosystem just can’t stop growing. Physicians’ offices generate patient data from labs, devices, test sites, and research facilities, even from in-home data (i.g personal fitness devices or any mobile app that a patient uses to help them manage their diseases).
Putting all of those data together and sharing them across so many disparate systems is critical for healthcare providers to ensure the successful care of an individual patient and improve the overall population’s health.
That being said, managing and integrating all of that data is quite complicated. Not to mention that you also have patient information being created, updated, and examined daily.
This is where interoperability comes in handy.
Simply put, interoperability is the ability to share information between systems and software applications to communicate and exchange data in meaningful ways. It’s all about ensuring that different systems can connect, fit together, and exchange data seamlessly.
As a healthcare provider, you need to exchange information with other providers to deliver effective and accurate patient care. And this can take various forms, such as exchanging records like lab results and immunization records or sharing medical records about referrals, discharge, and registrations.
After all, a patient is not just a heart, a hip, or even a heartbeat. To get the full picture, healthcare providers need multiple images from multiple sources.
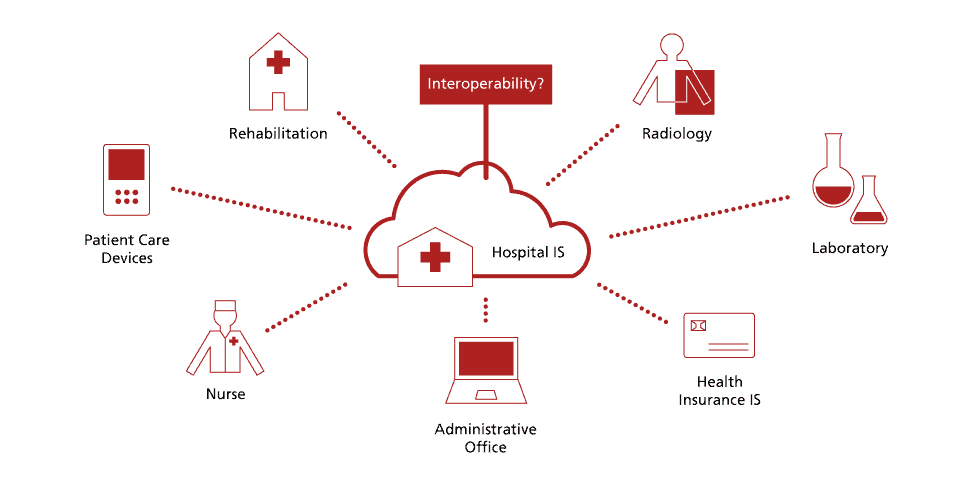
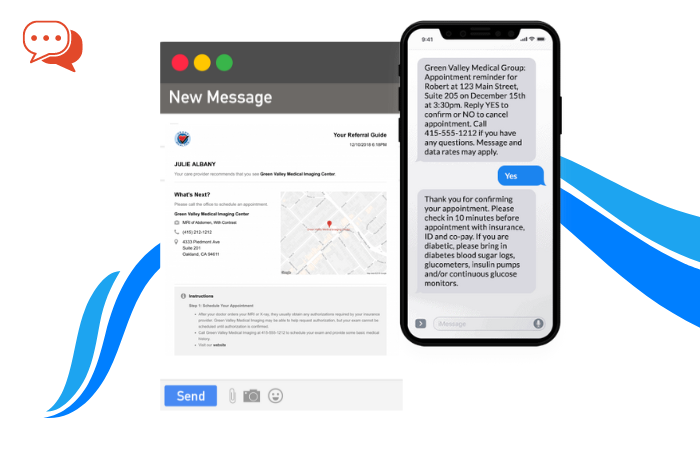
For instance, if a patient goes and has an x-ray in your local hospital, they have their blood pressure taken and checked by a nurse in the GP practice — or maybe they also need to provide data from their dietician.
All their data (collected by different professionals), rather than sitting in different systems and not being brought together, can be brought together in one single place with interoperability.
That integrated data exchange model enables all the information to be shared between healthcare providers, professionals, patients, hospitals, pharmacies, laboratories, etc., regardless of the application being used.
It helps healthcare providers make sure that they don’t have any isolated pockets of information about their patients that they miss since it can put patients and clinical facilities at risk.
In this case, advanced communication is a key benefit when it comes to interoperability. Different systems must be able to talk to each other for the best results. If systems are not interoperable, it’s almost impossible to decode the information to create meaningful patient data when data is sent from one system to another.
Why Is Interoperability in Healthcare Important?
Now that we know what interoperability in healthcare is all about, it’s time to understand what makes it so crucial for every healthcare provider. We’ve mentioned it slightly before, but now we’re going more in-depth.
In the healthcare industry, every piece of information collected needs to be distributed and recognized. That’s simply how the system works. This will help health information be accessed by healthcare professionals who need them, improving transparency, portability, and accessibility.
Gone are days when all that data-sharing happened via paper faxing and long phone calls. Not only does the old method eat up time and money on both ends of the relationship, but it also slows down the speed of a patient’s care.
Interoperability comes into play to make healthcare providers easily interact to share patient information, making health care data universally sharable. Therefore, all of the interoperability purposes boil down to one thing: easier data sharing and collaboration to achieve better health outcomes.
As you might already know, robust data sharing and improved collaboration allow better and more timely decision-making, particularly in critical situations. It means that if interoperability is not part of the equation, you make your patient’s health suffer even more.
So, if you ask: “how important is interoperability in the healthcare industry?” The answer is quite simple: It’s critical.
It allows patients and healthcare providers to access, input easily, and receive data. We can even say that interoperability is changing the climate of patient information technology forever.
Key Benefits of Interoperability in Healthcare
Interoperability makes data available whenever and wherever it is needed. This way, healthcare providers can make sure that they provide seamless medical care to patients. Even if patients are the ones who see the most benefits, interoperability also plays such significant role in helping staff do their tasks hassle-free.
To get a better picture, here are some essential reasons why interoperability has become necessary in today’s age:
Faster and More Accurate Patient Care
Interoperability in healthcare makes it easier for healthcare providers to share patient information data. They don’t have to perform redundant patient tests that might cost not only time but also money.
It also reduces the time it takes to have conversations and share insights between providers, doctors, and patients. This case enhances the healthcare delivery speed by making data easily shareable in a readable format.
Therefore, interoperability makes healthcare more efficient by helping specialists communicate quickly with referring doctors to get to the heart of the matter as they make decisions about treatment.
Better Patient Outcomes
Continuity of care is key in treating patients — especially for patients with chronic conditions or taking care of an acute situation that involves multiple health service providers.
Most patients have received different healthcare from different providers in their lives, such as clinics, independent practices, and hospitals. Those interactions make up the entirety of their medical history.
Interoperability helps healthcare providers gather all the information seamlessly even if the patient cannot provide all details of their medical history. This can result in a safer transition of care that can lead to a better patient outcome overall.
Score and Share Data Securely
Protecting patients’ information and their sensitive data must be one of every health care’s top priority.
As a healthcare provider, you know the care you provide doesn’t start and stop when a patient comes to see you. You have a responsibility to ensure that the trust they put in you by giving you their information is kept safe and secure.
With interoperability, only a few people can touch and make changes to patients’ data. This way, there’s less chance for that data to go astray and get attacked by criminal hackers. Your IT department can limit people who have full access to the data so that it would be much easier to monitor staff compliance.
Improves Staff Productivity
Besides its advantages to performing a better service and improved accuracy to treat patients, interoperability also helps healthcare providers to improve their staff productivity.
Working with interoperability means that you don’t have to take too much time typing and input the same information repeatedly since you can access the detail or previous records you need in the Electronic Health Record or EHR system.
Spending too much time on tasks such as entering or searching for patient data makes staff don’t have much time to deliver care. Interoperability helps staff save time in finding and updating records, which means they have more time to focus on increasing margins by treating more patients and improving their quality of care.
Give Patients Better Experience
With interoperability, your patients no longer need to fill the same repetitive forms to give you details about their medical history. They also do not need to spend too much time explaining their conditions or situations. All of their details and medical records are stored in one place so that the staff can easily before consultation or follow-up.
The medical staff that can see the details and the patient is also allowed to understand all of your medical history and records. And when patients have easy access to their medical records, they can be more informed and more active or fully participate in decision-making. This easier method can surely increase your patients’ overall experience and satisfaction.
Provide Better Data Exchange With Other Systems
You can easily communicate with other providers or services that your patients have worked with before using interoperability. So, it’s easy for your patient or medical professionals to understand your patients’ conditions and treat them accurately.
In other words, it reduces the time-consuming document-based information exchange between systems by feeding the information directly into workflows.
Interoperability also makes it easier for you to communicate digitally with their pharmacists. The pharmacist doesn’t have to try so hard to decipher the doctor’s handwriting since they can send out a digital version. The prescriptions will be sent out to the pharmacy before the patient has even left the waiting room.
Prevent Data Errors
Medical errors are costly, no matter where they occur. Small, tiny mistakes might not be life and death, but they can still impact healthcare providers and sometimes even interrupt some operations.
Those errors often occur because of unmade updates, incomplete or missing patient data, or any issues with data entry. In this case, every healthcare provider should treat their patients and capture and process data across the systems without all the red tape and delays.
Interoperability helps you avoid those critical data errors since it stores data on EHR that is easy to update in real-time. It also prevents administrative errors and prescription making, making it easier for doctors to make decisions faster and better.
Create Better Public Health Data
Multiple streams of data and disparate systems can cause problems when it comes to public health. Interoperability ensures that all electronic health information is shared appropriately and effectively between healthcare and public health partners.
Interoperability also provides healthcare providers and all stakeholders with a transparent, accurate view of a public health crisis. This way, they can recommend better and relevant guidelines for the public. This, in turn, will help create better public health.
More Autonomy in the Recovery Process
Interoperability also allows more autonomy in the recovery or therapeutic process. Patients will have more control over their own data, eliminating a significant amount of that administrative burden.
Also, especially for patients who suffer from chronic disease, access and tracking their medical status and progress is critical. It will help them stay motivated for the recovery, but it will also help them develop a more active role in their healthcare and a greater self-management.
Bringing Down National Healthcare Costs
The redundancy of lab tests that have to be done because of lack of crucial information flow will waste time and lead to a pretty large increase in healthcare costs.
Interoperability is an underlying tool that is meant to streamline care by putting all data in one place. And if all the data is stored and available in one place, healthcare providers can avoid unnecessary repeat testing and preventable adverse drug events, reducing national healthcare costs.
According to the report, interoperability has been proven to save at least 77.8 billion dollars per year in the United States. Of course, to maintain this number and keep making this benefit happen effectively, it is up to healthcare providers, third-party app developers, and payers.
Implementing Interoperability: The Challenges
Now that we’ve broken down some key advantages of interoperability, it should be clear that this healthcare innovation can benefit healthcare providers and patients. Therefore, interoperability has now become a must-have for healthcare providers around the world.
The current lack of interoperability in healthcare can compromise patient safety, contribute to clinician burnout and task overload, and of course, waste billions of dollars a year. It should come as no surprise that EHR/EMR system spending just keeps increasing each year — at least in the United States. The report from eMarketer says that the US will spend nearly $16 billion on electronic health record (EHR) and electronic medical record (EMR) systems in 2022.
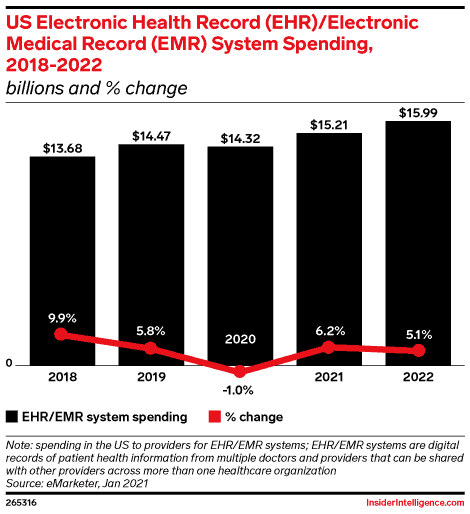
However, one-third of health systems still struggle with interoperability implementation today besides all those benefits mentioned above. They claim that their interoperability efforts are insufficient. And one of the main reasons is the lack of standards for sending, receiving, and managing information between health systems.
There is no interoperability standard. In this situation, it’s critical to find more efficient ways to find and see the convergence toward some common standards. This way, all the health systems can seamlessly connect fragmented patient data in the future and implement better and more accessible interoperability.
With some effort, though, interoperability can and will be achieved by all the healthcare systems worldwide. But, like all things, a good deal of time and energy is required.
For interoperability to help improve healthcare systems and tackle its own challenges, clinical data needs to be ensured to flow freely across networks in the first place.
Since there is still a lot of room for improvements, we know that health systems, payers, providers, and hospitals are constantly seeking innovation when it comes to more effective and efficient interoperability. It means that interoperability in healthcare will always continue to evolve and improve as new advancements in technology are made.
Final Thoughts
Sharing patients’ clinical information is not new. Interoperability has been the Achilles heel in healthcare data for quite some time. Thanks to them, patients now can get a more convenient healthcare experience and enjoy better protection and safety. After all, improving the patient experience will depend on hospitals’ ability to integrate healthcare data and IT systems with interoperability. With this advanced technology, the staff and healthcare providers also make the most of their time and reduce costs when giving the best service.
As interoperability shifts from being a theoretical goal in the healthcare industry to a practical necessity, every healthcare provider worldwide are strongly encouraged to implement them to make fully informed care decisions.