Strokes happen fast–in as little as 15 minutes. To be sure, even the language in top medical reports on the subject speak of strokes as “sudden attacks,” which happen so acutely that over ten million people worldwide die or are permanently disabled by them each year. It’s a problem that’s plagued healthcare efforts for decades, with EMS professionals being the last line of defense to detect stroke symptoms pre-hospital.
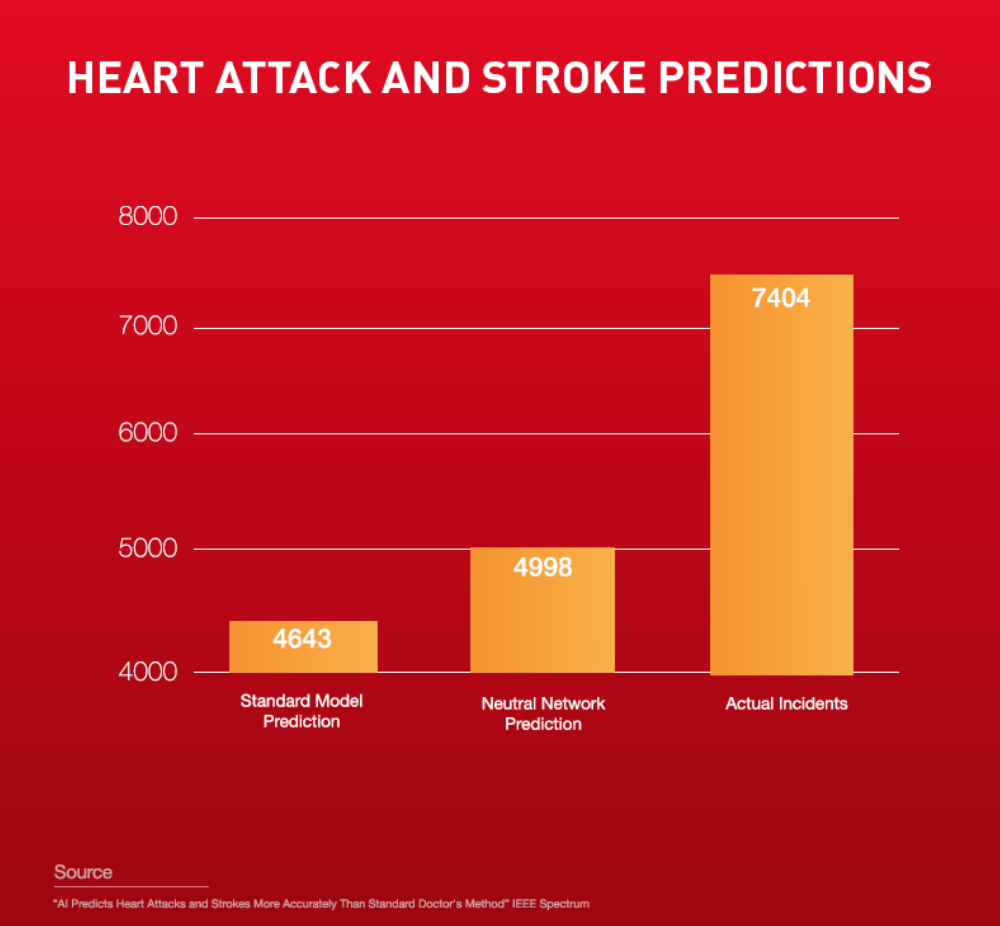
These days, taking a predictive approach to preventing the severity of a stroke has become a lot more feasible thanks to intensive research and testing into how Artificial Intelligence (AI) technologies might be best deployed in a healthcare setting. Researchers have even gone as far as developing machine learning. Natural language processing algorithms that have (in one 2017 trial, more accurately than doctors) predicted which patients will suffer a stroke within a decade.
Exploring Artificial Intelligence and Stroke Response
In light of these technological advancements, this article sets out to explore and capture how today’s AI systems have been developed to optimize a practitioner’s ability (regardless of their neurological training) to predict or detect the signs of stroke prehospital.
First, we’ll talk about the importance of (and difficulties associated with) early stroke diagnosis. Next, we’ll summarize the current context of today’s healthcare AI technologies and how they work, then expanding on how these systems are changing the face of stroke-related care today to talk about what’s next for AI’s use in stroke detection.
Note: This assessment focuses largely on the ability of AI systems to detect or predict the precursors for Ischemic stroke (as opposed to Hemorrhagic stroke), which makes up over 85% of stroke cases, and for which the most Electronic Health Record (EHR) data is available.
Why is it so hard to predict and detect stroke?
Up to now, there have been very few reliable biomarkers that help neurologists distinguish which patients will suffer from a stroke in the future. And although years of clinical research trials have yielded positive results about the subject, a general lag in the evolution of healthcare IoT infrastructures has continued to limit the replicability of such studies, especially given the sheer amount and complexity of patient data needed to provide significant analyses of these markers.
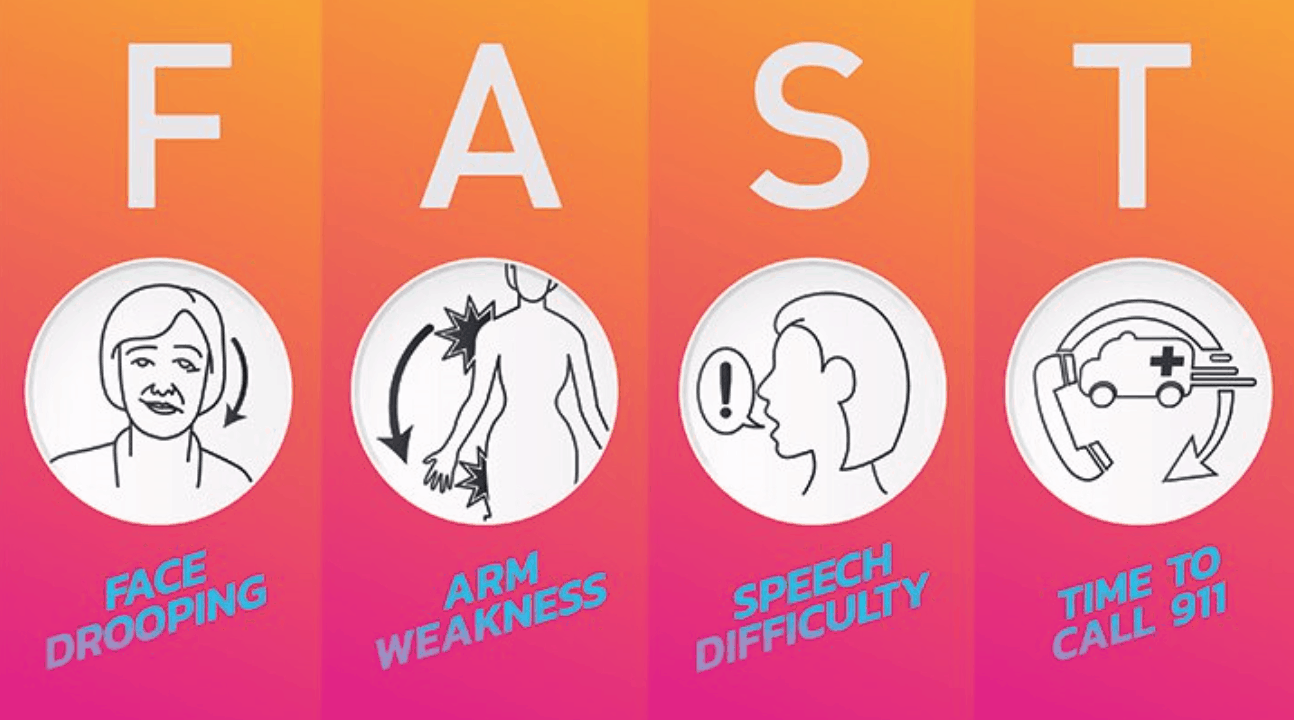
Available retroactive data has, of course, given physicians and neurologists cues about which patients might be more at risk for stroke. However, actually moving to the diagnosis stage largely occurs while a stroke is happening. Therefore, current stroke response procedures often involve on-the-spot testing with EMS professionals or paramedics who may check for physical stroke predictors like facial weakness or slurring of speech by asking patients to smile or by running them through a set of simple questions.
To some, these physical measures may seem quite latent–especially since EMS first-responders have been found to offer a compassionate diagnosis of acute stroke patients. Yet a continuing gap in the efficiency of prehospital stroke diagnosis (in a similar study, correctly identifying stroke only 52% of the time, with paramedics identifying at 72%) disproves that confidence and often results in delay critical patient care.
The importance of predicting an Ischemic stroke early.
This delay is particularly concerning when we consider that Ischemic stroke patients suffer the loss of two million brain cells every minute until blood flow is restored. In this context, an earlier diagnosis can mean faster treatment, with one Harvard Medical study breaking down the benefits as follows:
“For every 15-minute acceleration of time to…treatment, [researchers] found:
- 4% lower risk of in-hospital death
- 4% better odds of walking independently after leaving the hospital
- 3% better odds of being sent home instead of to an institution
- 4% lower odds of a brain hemorrhage.”
Translation? Earlier stroke recognition significantly improves patient outcomes.
Technological Responses to Stroke Detection
Given the inherent rewards involved in diagnosing a stroke early, biotechnologists and other clinical researchers have long committed to developing the technological means to empower first responders and other non-neurologists incorrectly detecting the signs of a stroke. These diligent efforts have managed to decrease one-year mortality following stroke by 23% or more from creating stroke units and rolling out stroke-response metrics and training.
In the last few decades, though, some technological healthcare advances – such as the widespread deployment of Electronic Health Record systems and subsequent advancements in computing power for data processing and telemedicine – have laid the foundation for the next generation in predictive stroke technology: Artificial Intelligence.
Artificial Intelligence in Healthcare: How Does it Work?
Like any good scientist, AI systems are based on machine learning or natural language processing algorithms that can ‘understand’ vast amounts of relevant data with life-like speed, recognizing patterns or creating a kind of ‘logic’ based on the information given. These supervised ‘learning’ sessions are often guided or programmed by an algorithm’s creator. Once complete, researchers can then use the resultant software to different input data into sets, according to any of the parameters they need to examine.
These technologies have thus found an appropriately vast number of applications in a healthcare setting. In these cases, AI systems are ‘trained’ on data generated via regular clinical proceedings and quantified from medical notes, electronic healthcare device recordings, clinical laboratory studies, and many other sources, only later put to task assisting researchers and practitioners in revealing clinically relevant information hidden in large quantities of patient data.
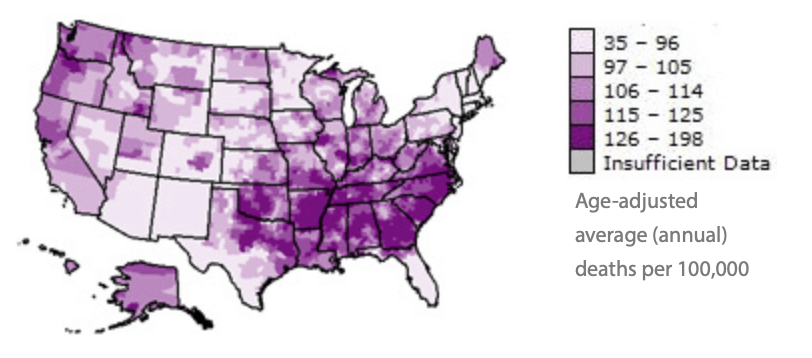
U.S. Stroke Deaths 35+, 2000–2006, by County
It has thus been the fusion of an increasingly large database of readily available patient health information paired with AI technology’s potential in solving stroke’s critical time problem – a problem keeping stroke as one of the leading causes of death in the US, resulting in almost 140,000 deaths per year – that has continued to draw clinical researchers to studying predictive stroke measures at the intersection of AI.
How AI Can Predict and Detect Stroke
Given that neuroimaging techniques like Magnetic Resonance Imaging (MRI) or Computed Tomography (CT) scans are most often used to identify stroke, researchers have created assistive AI tools that respond to or analyze these machines’ informatics and imaging outputs in particular. From there, deeper retroactive analyses can be made into the neurological symptoms of studied stroke patients, offering greater clinical insight into the kinds of biomarkers that may correlate with the occurrence of stroke. In other cases, an algorithm can quickly assess images from MRI or CT scans, signaling to a stroke specialist in-hospital (or remotely). Patients require immediate care.
Within this context, AI systems and their associated algorithms can be deployed either at the clinical research stage or at a physician’s point of care. In either circumstance, medical professionals are trying to detect the symptoms of a stroke prehospital, with the ultimate goal of being able to predict who is most susceptible to stroke accurately and equipping them with technologies that can notify a physician of a potential stroke in their patients, long before it has the chance to occur.
In support of these technologies, quite a few clinical studies have been conducted, which further affirm the potential success of both research and bedside stroke response systems. For example, a related study by Gupta et al. notes, “Artificial Intelligence offers technology solutions with high precision and accuracy for the diagnosis of stroke, its severity as well as prediction of functional outcomes,” with a similar study endorsing the same, saying: “AI techniques in stroke imaging could markedly change…stroke diagnosis and management in the future…[and] machine-based diagnosis would be beneficial for medical staff who are not accustomed to stroke imaging.”
A real-world example of how AI can predict and detect stroke
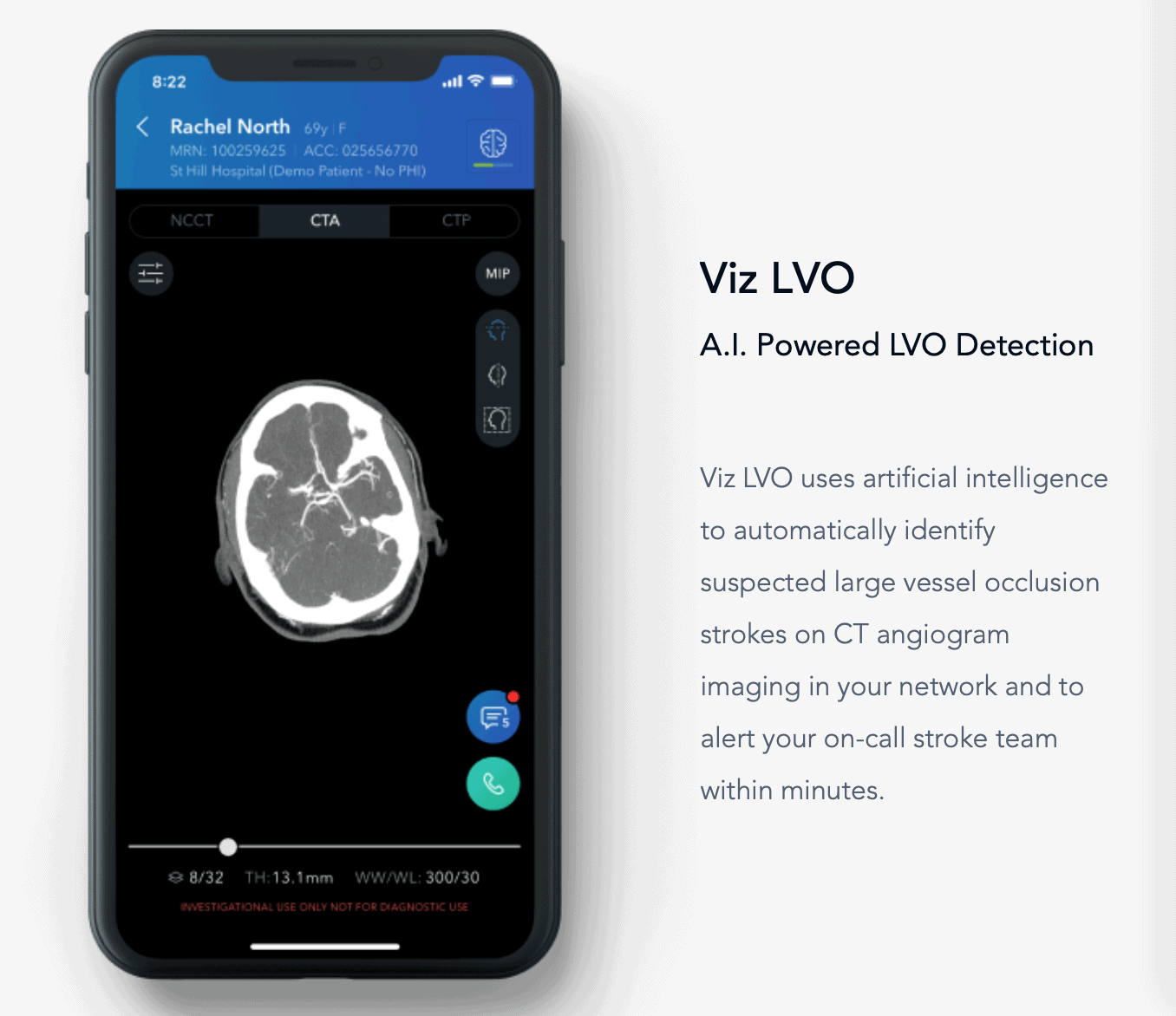
To better break down how AI technologies are being used to predict and detect stroke, let’s point to the example of Viz.ai, who recently partnered with Medtronic to deliver their artificial intelligence ‘contacts system’ to stroke care centers across the greater US.
Recently gaining FDA clearance, Viz.ai’s software has been developed to sync up with CT scanners and is already performing well in hospitals all over the US. Their software uses advanced deep learning, sending radiological images directly to a stroke specialist’s smartphone, helping them diagnose high-risk patients from anywhere in the world.
As a result, Viz.ai has been able to leverage artificial intelligence to – quoting their website – “synchronize stroke care, reducing systemic delays that stand between patients and life-saving treatments.” With the built software designed to engage in preliminary diagnoses and stroke patient triage, Viz.ai’s artificial intelligence can even detect suspected large vessel occlusion (LVO)–a common predictor or symptom of Ischemic stroke. In fact, according to a study they conducted, later reported through the Medical Device Network, “Viz LVO demonstrated the ability to alert the stroke specialist earlier than standard in 95.5% of true positive cases…sav[ing] an average of 52 minutes.”
Other companies using AI to predict and detect stroke
These developments in responsive (and even predictive) stroke care have been welcome news for medical professionals at all levels, with other frequent successes still on the rise at the intersection of AI systems and healthcare, particularly for early stroke detection and prediction.
For instance, iRAPID uses AI technology to “expand the treatment window for neurovascular conditions” through real-time views of brain perfusion and is a technology that has found a home in over 1300 hospitals globally. NeuroView, a medical technology startup, is also aiming to “automate the detection of stroke deficits to make better predictions about stroke in the field,” a goal echoed by many of today’s most recognized medical associations, healthcare technology companies, and even hospitals who are notably teaming up to tackle similar problems, building their own AI systems for department and consumer use.
The limitations for AI technology and stroke prediction
Of course, the work here is never done. Given the proven potential for success, healthcare companies and other healthcare innovation organizations have been forced to answer the difficult question of whether AI algorithms are sophisticated enough to mimic the complex medical decision-making problems involved in stroke care.
With these technologies only recently entering widespread implementation, it will take some time before AI accuracy outshines that of actual practitioners–meaning neurologists aren’t about to lose their place in stroke-care processing. Even NeuroView, mentioned above, admits that although they successfully developed an algorithm that can recognize facial weakness in standard video with 89% accuracy, that their “algorithm’s accuracy did not significantly differ from the average accuracy of EMS providers in [, they are] study.”
A similar report from the American Health Association echoes these sentiments, admitting that further research is still needed generally, and concerning the subject of their study, to “refine” stroke-detecting algorithms and expand them to detect other stroke deficits “such as limb weakness and ataxia.”
AI technology and stroke: Forecasts for future success
Regardless, the leaps and bounds that researchers have made in the last decade alone can’t be ignored, largely casting a positive forecast for what healthcare practitioners, patients, and businesses can expect to see in the future of healthcare AI in general and the early prediction and detection of imminent stroke in the specific.
While imaging interpretation, tissue mapping, and telecommunication applications continue to evolve at the intersection of Healthcare AI, further explorations will have to surmount the difficulties of replicating the often chaotic, erratic clinical decision-making process involved in diagnosing stroke.
And yet, in light of what we’ve already explored, including the process of digital stroke response and why it remains so difficult in today’s technological economy, we’ve seen what some of healthcare’s greatest minds have been able to accomplish amid these high-stakes conditions, and have gained a researcher’s mindset in understanding where stand, and where we are going as we continue to explore AI technology and its applications in predicting and detecting stroke.