Conventional medical care consists of patients being treated at hospitals or care centers when they are sick, injured, or dying. In a sense, this is a reactive solution in regards to the issue of health. The problem is that routine checkups and screenings are essentially voluntary. Only once a malady or injury has already occurred does a person receive medical attention.
In recent years, there has been a renewed emphasis on preventive health, specifically immunizations and screening tests. Indeed, most health insurance plans now cover these preventive services.
For a full list of preventive care benefits covered by health plans, click here.
Teach Patients To Be Proactive, Not Reactive
One important aspect of preventive medicine is lifestyle change with regards to diet, alcohol, drugs, sexual activity, etc. The fact that adjustments in lifestyle can have such a profound impact on health has led to some hospitals and health centers reaching out to their respective communities in order to address social and environmental factors that can impact health. The actions of these proactive organizations has led to a newfound emphasis on the health management of populations.

What Is Population Health?
 Population health is defined as “the health outcomes of a group of individuals, including the distribution of such outcomes within the group.” (Source)
Population health is defined as “the health outcomes of a group of individuals, including the distribution of such outcomes within the group.” (Source)
The goal of population health is to reduce health inequalities and gaps among different populations. This is usually done by addressing the social determinants of health (SDOH), which are commonly thought of as the social and economic factors distributed among a population that affect differences in health status.
These are not individual risk factors like genetic makeup, but instead are things like the distribution of wealth among a population. The idea is that health begins in our communities, whether that means at home, school, work, or elsewhere. It is in these settings where people practice healthy habits, such as eating right, being active, not smoking, getting immunizations and screenings, etc. Unfortunately, not all people have access to the same opportunities or resources, and this is the reason that such health disparities exist.
Why Exactly Do Health Disparities Exist?
There are varying reasons for these inequalities, chief of them being certain political ideologies that lead to poor public and social policies. These policies tend to shape the social and economic environments that affect a population’s health.
The following organizing framework was developed by Healthy People 2020 in conjunction with the Center for Disease Control and Prevention and the Office of Disease Prevention and Health Promotion. Click here to learn more about the full initiative.
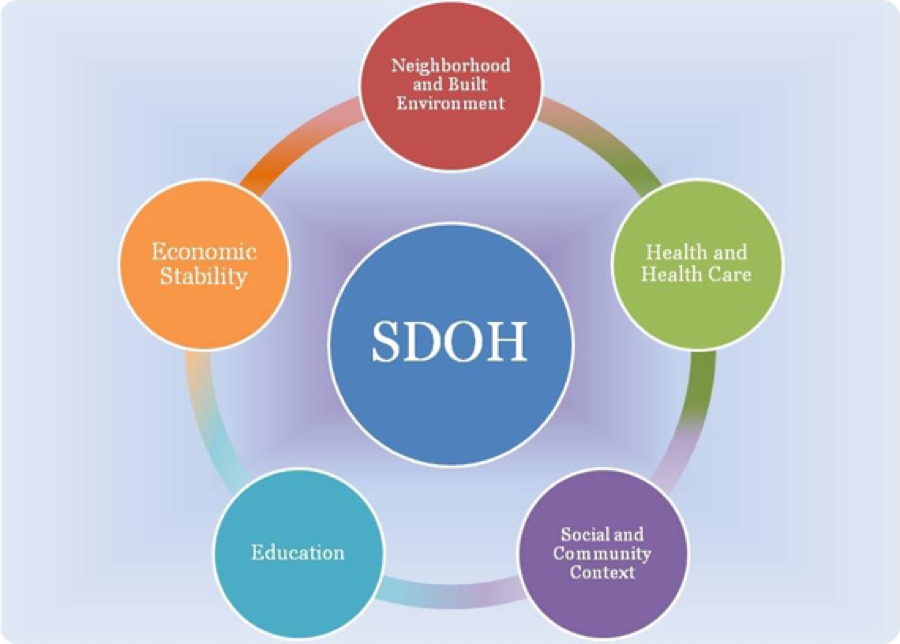
There are five overarching social determinants of health.
And within each of these five broad categories, there are more underlying factors that contribute to health disparities.
- Education

- High School Graduation
- Higher Education Status
- Language & Literacy
- Childhood Development and Education
- Economic Stability

- Poverty
- Employment
- Food Security
- Housing Stability
- Social and Community Context

- Social Cohesion
- Civic Participation
- Discrimination
- Incarceration
- Neighborhood and Built Environment

- Access to Healthy Food
- Housing Quality
- Violence & Crime
- Environment
- Health and Health Care

- Access to Health Care
- Access to Primary Care
- Health Literacy
The growing evidence that one’s health can be attributed to social, behavioral, and environmental factors is unmistakable.
So much so that the World Health Organization (WHO) put out a list of action areas and case studies that serve as proof of the impact that social determinants on health have globally. The WHO focuses on nine broad areas with their global plan and initiatives.
These are listed below:
- Employment Conditions

- Social Exclusion
- Priority Public Health Conditions
- Women and Gender Equity
- Early Child Development
- Globalization
- Health Systems
- Measurement and Evidence
- Urbanization
To learn more about these social determinants of health and the evidence behind them, you can click here.
Additionally, there are countless public health studies, reports, and publications that all prove the importance of these socioeconomic factors on health.
Take this study published in Public Health Reports. It provides strong evidence that income, wealth, education, and other socioeconomic issues are fundamental to health outcomes. Here’s a little sample:

We can clearly see that there is a strong case for hospitals to engage in community health management.
Who Is Currently Doing It?
Some hospitals and health centers are choosing to embrace population health initiatives.
Most of these organizations tend to take two steps before strategically going about tackling the underlying factors that lead to poor community health outcomes. These steps are:
![]()
- Broadening target population and strategic region to not only include potential patients but also the entire geographic region

- Partnering with local and federal organizations to help implement programs targeting socioeconomic factors
With the first step, it is important that the healthcare system takes an organization-wide approach to expanding its scope and mission to include impacting social determinants of health throughout its geographic community.
 Accountable Care Organizations (ACOs), for example, are incentivized to participate in community health initiatives. These organizations prescribe to value-based care models and risk sharing health plans, making them responsible for the health costs that their patients incur. This is why they are encouraged to improve the socioeconomic landscape, and as a result the overall health, of their communities.
Accountable Care Organizations (ACOs), for example, are incentivized to participate in community health initiatives. These organizations prescribe to value-based care models and risk sharing health plans, making them responsible for the health costs that their patients incur. This is why they are encouraged to improve the socioeconomic landscape, and as a result the overall health, of their communities.
Click here to learn more about the Accountable Health Communities Model.
Kaiser Permanente, for example, is very committed to improving the health of its community. According to their 2014 Community Benefit Snapshot, they:
- Invested over $2.2 billion into the community – people, environment, knowledge, etc.
- Taught nearly a million students about healthy eating, exercise, and sexuality through music, drama, and comedy
- Sponsored over 50 local farmers’ markets throughout the country
- Published over 1300 articles in scholarly journals (Source)

Due to them being beneficiaries of an estimated $24.6 billion tax exemption in 2011 (Source), nonprofit hospitals and health centers are required by the government to partake in community benefit activities. The Affordable Care Act has put into place legislation obligating these institutions to participate in projects or programs that aim to improve the overall health of their respective communities.
 For example, Mount Sinai Hospital in New York City is one of the largest nonprofit hospitals in the country. They pride themselves in having a vast population outreach program. You can see their various community health centers and initiatives here.
For example, Mount Sinai Hospital in New York City is one of the largest nonprofit hospitals in the country. They pride themselves in having a vast population outreach program. You can see their various community health centers and initiatives here.
The Martha Stewart Center for Living at Mount Sinai, and the Linkage Houses, are two of the more successful community health programs for the elderly in New York City. The Linkage House offers safe and affordable housing, while the Martha Stewart Center provides healthy living activities and educational programs/resources.
Learn more about nonprofit hospitals’ community benefit requirements here.
The second step eases the financial burden on the health system by allowing them to partner with community or government organizations that are initiating, or already have established, programs that address these socioeconomic disparities. For example, there are many nationally funded programs that seek to improve access to healthy food, better housing, better schools, etc. Hospitals can choose to be a part of those programs by investing resources and personnel into them.
The Center for Disease Control and Prevention sponsors a variety of national health initiatives that target socioeconomic factors in the hopes of improving public health. Here is a list of areas that they focus on:
Even states, like New York, take it upon themselves to invest in programs that unite healthcare institutions and community organizations to cooperate on population health initiatives.
Learn more about the New York State Health Improvement Plan here.
How Are They Doing It?
![]() It all starts with leadership. Hospitals that employ physician leaders passionate about addressing all aspects of health are more likely to find themselves engaged in population and community health programs. With the emergence of value-based care models, more and more executives are choosing to allocate funding and resources to these programs in the hopes that they will eventually lead to lower healthcare costs and better healthcare outcomes in the future.
It all starts with leadership. Hospitals that employ physician leaders passionate about addressing all aspects of health are more likely to find themselves engaged in population and community health programs. With the emergence of value-based care models, more and more executives are choosing to allocate funding and resources to these programs in the hopes that they will eventually lead to lower healthcare costs and better healthcare outcomes in the future.
Many CEOs are choosing to align the mission of the hospital (if it is not already) towards community service and engagement. This allows for a clear and concise purpose to be known throughout the organization. All staff and employees will know to abide and perform towards the ultimate overarching standard. This is especially important in disadvantaged communities, as these are areas where socioeconomic factors tend to play a huge role in the overall fitness of that population. Having a healthcare institution committed to improving the well-being of a community is one of the most powerful resources that a population can have. Even more so when that institution is able to partner with existing and emerging federal (or private) organizations that are out to better the health of a community.
Some examples of great community projects and initiatives that have had a direct impact on improving people’s health include:
- Affordable low income housing in safe or rehabilitated neighborhoods
- Access to healthy foods (through collaboration with local farmers and grocery stores)
- Build parks, gardens, recreation centers
- Support local education and employment initiatives

All of these projects and programs are not possible without financial and human resources. Many hospitals do not receive the proper funding needed or have the personnel available for community health engagement. Therefore, it is even more important for these institutions to seek out partnerships with existing organizations that are successful in their initiatives. This means local schools and businesses. This means local government and nonprofits in the area. Without outside help, hospitals will have a hard time devoting enough time and manpower to make a real impact on the socioeconomic landscape of their community.
![]() However, when they do make investments into community health programs, hospitals and health systems desire to monitor the progress of their involvement. They need a way to measure the improvements in health and cost that are direct results of these community initiatives. The best way to do this is to enhance the existing EHR software to track socioeconomic factors of health and be able to share this data throughout the community. This ensures transparency and clear communication between the hospital and the primary care or specialist physicians in the community.
However, when they do make investments into community health programs, hospitals and health systems desire to monitor the progress of their involvement. They need a way to measure the improvements in health and cost that are direct results of these community initiatives. The best way to do this is to enhance the existing EHR software to track socioeconomic factors of health and be able to share this data throughout the community. This ensures transparency and clear communication between the hospital and the primary care or specialist physicians in the community.
 This is of utmost importance to making sure that community health programs are having a positive effect. Primary care physicians are the first line of communication for patients and it is with them that healthy habits and home life are discussed. Therefore, PCPs are some of the best resources for hospitals to learn about the health of their community and the socioeconomic environment that their patients live in. This information can help direct organizations towards what programs will be beneficial to their respective target populations.
This is of utmost importance to making sure that community health programs are having a positive effect. Primary care physicians are the first line of communication for patients and it is with them that healthy habits and home life are discussed. Therefore, PCPs are some of the best resources for hospitals to learn about the health of their community and the socioeconomic environment that their patients live in. This information can help direct organizations towards what programs will be beneficial to their respective target populations.
referralMD helps connect hospitals to the community. Our real time, HIPAA compliant, communication platform allows for improved care and increased transparency all along a patient’s care continuum. Health providers are able to easily view a patient’s medical history and even customize their referral forms to include certain social or economic factors that could affect that patient’s health. Indeed, hospitals can establish an organization-wide emphasis on population health by having all referring providers (within and outside of the network) complete referral forms that list various social determinants of health and lifestyle habits/changes. Our platform allows health systems the freedom to do this and encourages referring providers to follow through.
 Request a demo today to learn more about referralMD’s HIPAA-compliant collaboration and communication referral management platform.
Request a demo today to learn more about referralMD’s HIPAA-compliant collaboration and communication referral management platform.